PCOS – Symptoms, Causes & Treatment in Women: Everything You Need to Know

What Exactly Is PCOS — and Why Is It So Common Now?
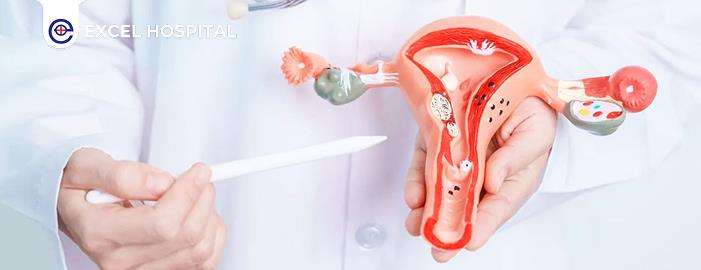
PCOS — Polycystic Ovary Syndrome — is a hormonal disorder where the ovaries produce an excess of androgens (male hormones). This hormonal imbalance interferes with the normal development and release of eggs during the menstrual cycle. Instead of being released, eggs may develop into small fluid-filled sacs (follicles) on the ovaries — giving the condition its name.
But here’s something most people don’t realise: you don’t actually need to have “cysts” on your ovaries to be diagnosed with PCOS. The diagnosis is based on a combination of symptoms, blood tests, and ultrasound findings — not cysts alone.
What makes PCOS so relevant today is the pace at which it’s growing. Sedentary lifestyles, processed food diets, chronic stress, and rising rates of insulin resistance have all contributed to making PCOS one of the most commonly diagnosed conditions among women of reproductive age across India — particularly in urban settings.
According to the World Health Organization (WHO), PCOS affects an estimated 8–13% of women of reproductive age globally — and in India, several studies suggest the prevalence is even higher, particularly in urban populations.
Diagram: A normal ovary releases a mature egg each month. In PCOS, multiple immature follicles accumulate — ovulation is irregular or absent
Symptoms of PCOS — Not Every Woman Looks the Same
PCOS affects multiple systems simultaneously — skin, hair, weight, hormones, mood, and fertility
One of the reasons PCOS goes undiagnosed for so long is that it doesn’t look the same in every woman. Some women have all the classic signs. Others have just one or two that they’ve been writing off for years. Here are the symptoms you need to know:
Fewer than 8 periods a year, very long gaps between periods, or periods that simply stop — are among the most common and earliest signs of PCOS-related ovulation disruption.
Especially around the abdomen and waist — even without major changes in diet. This is driven by insulin resistance, which is present in up to 70% of women with PCOS.
Excess androgens cause the hair follicles on the scalp to shrink, leading to thinning or male-pattern hair loss — which can be emotionally distressing and often the first sign women notice.
Growth of coarse, dark hair on the face, chest, stomach, or back — caused by elevated androgen levels. This affects up to 70% of women with PCOS and can significantly impact self-esteem.
Hormonal acne in PCOS tends to appear along the jawline, chin, and lower cheeks. It is often cystic, persistent, and doesn’t respond to typical over-the-counter skincare products.
Since PCOS interferes with regular ovulation, conception becomes more difficult. PCOS is the single most common cause of anovulatory infertility — but it is also one of the most treatable.
Hormonal fluctuations in PCOS have a direct effect on brain chemistry. Studies show women with PCOS have significantly higher rates of anxiety, depression, and low self-esteem — yet mental health is rarely addressed in routine PCOS management.
Dark, velvety patches of skin — typically on the neck, armpits, groin, or under the breasts — are a visible sign of insulin resistance, which often accompanies PCOS.
What Causes PCOS? It’s More Than Just Hormones
PCOS doesn’t have a single, clear-cut cause — it’s a combination of genetic, hormonal, and lifestyle factors that interact with each other. Understanding the causes helps you understand why treatment needs to be multifaceted, not one-dimensional.
The most significant contributing factor in most women with PCOS. When cells stop responding to insulin efficiently, the pancreas produces more of it — and excess insulin signals the ovaries to produce more androgens. This creates the hormonal imbalance that drives many PCOS symptoms.
Elevated levels of male hormones (testosterone, DHEA) disrupt the normal menstrual cycle, prevent regular ovulation, and cause the physical symptoms of PCOS — including acne, hair loss, and hirsutism.
PCOS runs in families. If your mother, sister, or aunt has PCOS, irregular periods, or type 2 diabetes, your own risk is significantly higher. Multiple genes are thought to be involved — making it a polygenic condition.
Research shows that women with PCOS often have a low-level, ongoing inflammatory state. This inflammation stimulates the ovaries to produce androgens and contributes to insulin resistance — creating a feedback loop that sustains the condition.
Sedentary lifestyle, poor diet high in refined carbohydrates and sugar, chronic stress, and disrupted sleep all worsen insulin resistance and hormonal imbalance. While these don’t cause PCOS alone, they can trigger it in genetically susceptible women and make it significantly harder to manage.
In PCOS, the pituitary gland often releases too much LH (luteinising hormone) relative to FSH (follicle-stimulating hormone). This abnormal ratio prevents follicles from maturing fully and releasing eggs — leading to anovulation and cyst formation.
PCOS and Its Long-Term Health Risks — Beyond Fertility
PCOS is not just about periods and pregnancy. If left unmanaged, it significantly raises the risk of several serious conditions:
| Long-Term Risk | Why PCOS Increases This Risk |
|---|---|
| Type 2 Diabetes | Insulin resistance in PCOS often progresses to full diabetes — up to 50% of women with PCOS develop type 2 diabetes by age 40 |
| Cardiovascular Disease | Excess androgens and insulin resistance increase cholesterol, blood pressure, and inflammation — all heart disease risk factors |
| Endometrial Cancer | Irregular or absent periods means the uterine lining isn’t shed regularly — over time, this buildup increases cancer risk |
| Sleep Apnoea | Obesity and hormonal imbalance in PCOS increase the risk of sleep apnoea — which in turn worsens insulin resistance |
| Mental Health Conditions | Anxiety, depression, and eating disorders are significantly more common in women with PCOS |
| Metabolic Syndrome | A cluster of high blood pressure, high blood sugar, excess belly fat, and abnormal cholesterol — common in unmanaged PCOS |
PCOS left unmanaged increases risk of multiple serious long-term conditions — all preventable with early treatment
How Is PCOS Diagnosed?
PCOS is diagnosed using what is called the Rotterdam Criteria — a woman needs at least 2 of the following 3 features to be diagnosed:
Rotterdam Criteria: A minimum of 2 out of 3 features must be present (after ruling out other causes) to confirm PCOS diagnosis
2. Clinical or biochemical signs of excess androgens — acne, hirsutism, hair loss, or elevated testosterone on blood tests
3. Polycystic ovaries on ultrasound — 12 or more small follicles in one or both ovaries, or enlarged ovarian volume
Any 2 of these 3, after ruling out other causes, confirms PCOS.
A complete evaluation at Excel Hospital typically includes:
| Investigation | What It Tells Us |
|---|---|
| Pelvic Ultrasound (TVS) | Checks ovarian size, follicle count, uterine lining thickness |
| Hormonal Blood Tests | LH, FSH, LH:FSH ratio, testosterone, DHEAS, prolactin, AMH |
| Thyroid Function Test (TSH) | Thyroid disorders mimic PCOS symptoms — must be ruled out |
| Fasting Glucose & Insulin | Evaluates insulin resistance and diabetes risk |
| Lipid Profile | Checks cholesterol levels for cardiovascular risk assessment |
| AMH (Anti-Müllerian Hormone) | Elevated in PCOS; also reflects ovarian reserve for fertility planning |
🔗 Women’s Care Services at Excel Hospital
PCOS Treatment — A Personalised, Not One-Size-Fits-All Approach


Here’s something your doctor should tell you upfront: there is no single “cure” for PCOS — but there are highly effective ways to manage it that make a real, measurable difference to your symptoms, fertility, and long-term health. Treatment is always tailored to what matters most to you right now.
A low-glycaemic diet, regular exercise (especially strength training and walking), and consistent sleep are not vague lifestyle advice — they are clinically proven to reduce insulin resistance, lower androgens, restore ovulation, and improve every PCOS symptom. Even a 5–10% reduction in body weight can restart regular periods in women with PCOS who are overweight.
Combined oral contraceptive pills are often prescribed to regulate periods, reduce androgen levels, and manage acne and hirsutism. Anti-androgen medications (like spironolactone) may be added for skin and hair concerns. These do not treat the root cause but provide symptomatic relief while lifestyle changes take effect.
Metformin is an insulin-sensitising medication that addresses one of the root drivers of PCOS. It helps regulate blood sugar, lower insulin levels, support weight loss, and in many women, restore more regular ovulation. It is especially effective in women with PCOS who also have insulin resistance or prediabetes.
For women trying to conceive, medications like letrozole or clomiphene are used to stimulate the ovaries to release eggs at the right time. Combined with pelvic ultrasound monitoring (follicular tracking), this significantly improves the chance of natural conception. IUI is an effective next step when ovulation induction alone is insufficient.
A minimally invasive surgical option for women with PCOS who haven’t responded to medication for ovulation induction. Small holes are made in the ovary using laser or diathermy to reduce androgen-producing tissue — often restoring natural ovulation for months to years after the procedure.
Often the most overlooked aspect of PCOS management. Given the significantly higher rates of anxiety and depression in women with PCOS, psychological support — including counselling, stress management, and in some cases medication — is an integral part of holistic, complete PCOS care.
Common PCOS Myths — Busted
There is so much misinformation around PCOS — on social media, in family circles, and even from well-meaning but uninformed sources. Let’s clear up the most damaging ones:
| ❌ Myth | ✅ Fact |
|---|---|
| PCOS means you can never get pregnant | PCOS is the most treatable cause of infertility. Most women with PCOS conceive with proper treatment |
| You need to have cysts to have PCOS | PCOS is a hormonal diagnosis — cysts are not always present, and their presence alone doesn’t confirm PCOS |
| Only overweight women get PCOS | Lean PCOS is real and common — many women with a healthy BMI are diagnosed with PCOS |
| PCOS goes away after pregnancy | PCOS is a lifelong condition. Pregnancy does not cure it, though symptoms may temporarily improve |
| The pill cures PCOS | The pill manages symptoms but does not treat the root cause. PCOS typically returns when the pill is stopped |
| PCOS is only a reproductive problem | PCOS is a metabolic condition with long-term implications for diabetes, heart health, and mental wellbeing |
When Should You Actually See a Gynaecologist for PCOS?
The honest answer is: sooner than you think. Most women with PCOS wait 2–3 years after noticing symptoms before seeking a formal diagnosis. That’s 2–3 years of unnecessary suffering — and missed opportunity to protect long-term health. See a specialist if:
| Your Situation | What to Do |
|---|---|
| Periods more than 35 days apart — or fewer than 8 per year | Book a gynaecology consultation now |
| Unexplained hair loss, unwanted facial hair, or persistent acne | Ask for hormonal blood tests |
| Difficulty conceiving after 6–12 months of trying | Seek a fertility evaluation — don’t wait longer |
| Family history of PCOS, diabetes, or irregular periods | Get a baseline evaluation even if symptom-free |
| Teenage daughter with very irregular periods | Early evaluation is important — PCOS can present in adolescence |
| Dark patches on skin or rapid weight gain around the waist | Get insulin resistance and hormonal panel checked |
Dr. Aarti Vazirani is known for her warm, attentive, and deeply empathetic approach to women’s health. Patients consistently describe her as someone who listens carefully, explains everything clearly, and makes you feel genuinely heard — especially important when dealing with a condition as complex and emotionally loaded as PCOS. She provides comprehensive PCOS care — from hormonal evaluation and lifestyle guidance to ovulation induction and fertility support — tailored entirely to each woman’s individual goals and concerns. Learn more about Dr. Aarti Vazirani →
You’ve Been Managing Symptoms Long Enough. Let’s Find Real Answers.
Whether you’re newly diagnosed, struggling to conceive, or simply tired of irregular periods and unexplained weight gain — book a PCOS consultation at Excel Hospital, Ahmedabad today. Get a proper diagnosis, a clear plan, and a specialist who actually listens.
📅 Book Your Consultation Now
📞 +91-84691 59595 | +91-79489 49595
📧 [email protected]
📍 206, Shivalik 2, Satellite, Ahmedabad — 132 Feet Ring Road
Frequently Asked Questions About PCOS
Medical Disclaimer: This article is for general health awareness and educational purposes only. It is not a substitute for professional medical advice, diagnosis, or treatment. Please consult a qualified gynaecologist for any personal health concerns related to PCOS or hormonal health. | © 2025 Excel Hospital, Ahmedabad. All Rights Reserved. | www.excelhospitals.com